For decades, Intrauterine Insemination (IUI) has served as one of the earliest medical interventions offered to patients trying to conceive. Positioned as a relatively simple, low-cost, and minimally invasive step before more complex treatments and interventions, IUI was designed to give sperm a ‘head start’ by placing it directly into the uterus around the time of ovulation. But despite its long-standing role in the fertility journey, IUI has seen little meaningful innovation over time. Success rates remain modest, and for many patients, the process can feel imprecise, leaving critical questions unanswered about whether sperm ever reaches the fallopian tube, where fertilization actually occurs.
As fertility science has rapidly advanced, particularly in areas like In Vitro Fertilization (IVF), the earlier stages of care have largely lagged behind. This has created a frustrating gap for patients: many find themselves cycling through multiple IUIs with limited insight or progress, only to be escalated to IVF, a far more intensive, expensive, and emotionally demanding process. For a growing number of people navigating fertility, the question isn’t just whether IVF works – it’s whether there should be a more effective, data-driven option before getting there.
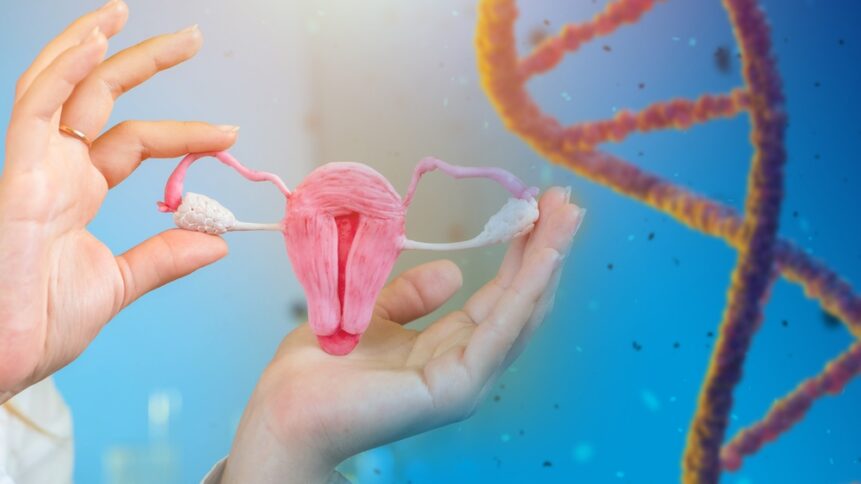
That’s where a new category is beginning to emerge. Known as Intratubal Insemination (ITI), this next-generation approach is designed to more closely mirror natural fertilization by placing sperm directly into the fallopian tube. Developed by Femasys®, FemaSeed ITI aims to bring greater precision, effectivity, and clinical insight to the earliest step of treatment, offering patients a modern alternative to traditional IUI. By rethinking where and how insemination occurs, this approach has the potential to redefine what a first step in fertility care can look like.
What Is IUI – and Why is the Success Rate Only 10-15%?
IUI works by placing washed sperm directly into the uterus around the time of ovulation, with the goal of giving sperm a shorter path to the egg. But while it bypasses the cervix, it still relies heavily on chance: sperm must travel through the uterine cavity, find the correct fallopian tube (where ovulation has occurred), and successfully fertilize the egg.
At each step, there are variables that can limit success, such as reduced sperm count or motility, timing challenges, or simply the fact that sperm may never reach the egg at all. Because IUI doesn’t control or confirm what happens beyond placement in the uterus, much of the process remains a black box, which helps explain why success rates tend to remain relatively low.
On a per-cycle basis, IUI success rates are typically cited in the range of 10-15% under optimal conditions, such as confirmed ovulation, open fallopian tubes, and adequate sperm count. In less ideal scenarios, those odds can drop into the single digits. While some patients do conceive through IUI, the majority will not achieve pregnancy in any given cycle – meaning many are advised to repeat the process multiple times to improve cumulative chances.
That repetition can come at a financial, physical, and emotional cost. Studies and clinical experience suggest that even after several cycles, cumulative success rates often plateau, with many patients ultimately needing to transition to more advanced treatments like IVF.
For patients, this can create a frustrating cycle of hope and disappointment, especially when each attempt offers limited insight into why it did or didn’t work. As a result, there’s growing conversation in the fertility space about whether IUI, in its current form, is truly serving patients as an effective first-line intervention, or whether there’s a need for more precise, data-driven options earlier in the journey.
The Vision Behind ITI: Meet the Inventor of FemaSeed®
Kathy Lee-Sepsick, CEO & Founder of Femasys, shares: “IUI has been around for a very long time – some have quoted for hundreds of years – and there hasn’t been any new innovation. That was the driving force to motivate me to take what we know should be a true first step in the fertility journey with insemination and make it better – specifically, looking at what natural fertilization requires, which is sperm meeting an egg in the fallopian tube. That’s what we do – we have a delivery platform that puts sperm directly into the fallopian tube. FemaSeed ITI is delivered similarly to an IUD or an IUI: through the vagina, through the cervix, and into the uterine cavity. Where we’re different is that we then utilize balloon catheter technology to isolate the opening of the fallopian tube to deposit the sperm directly to where it’s supposed to go.
FemaSeed is a first step and it’s done minimally invasively – there’s no surgery. Those elements are similar to IUI, but the key critical factor of having it enhance natural fertilization is what makes it different.
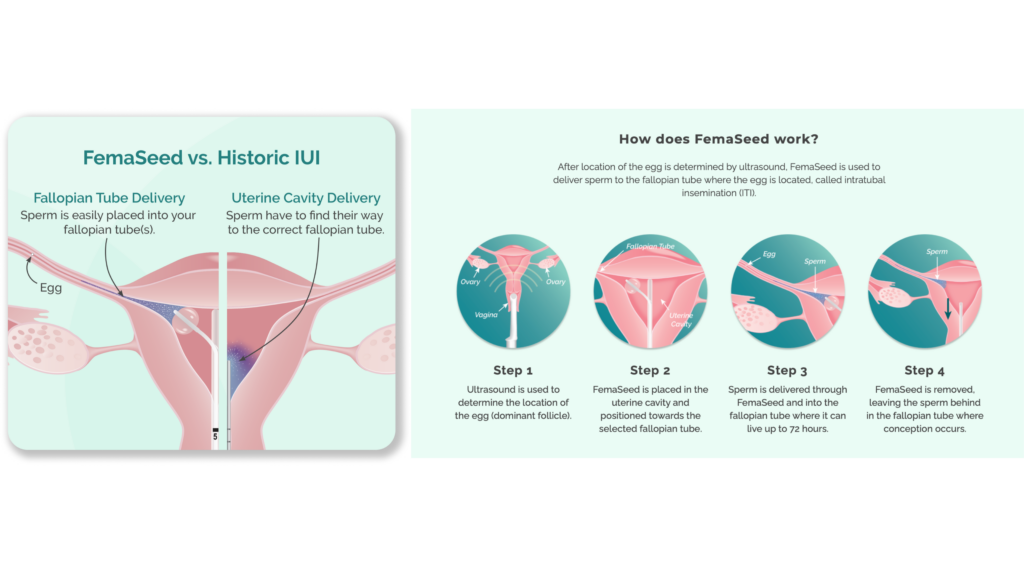
FemaSeed ITI is delivered similarly to an IUD or an IUI: through the vagina, through the cervix, and into the uterine cavity. Where we’re different is that we then utilize balloon catheter technology to isolate the opening of the fallopian tube to deposit the sperm directly to where it’s supposed to go. We’re taking the question mark off the table as to whether or not the sperm actually gets there, because we’re putting it right there exactly where it needs to go for fertilization.
Then the sperm still needs to do its own job, and the magic still needs to happen as far as fertilization and then the egg coming down and attaching to the uterine cavity into the endometrium. But we’ve extended the IUI process further by precisely placing the sperm into the tube.
Just because someone has a failed IUI does not mean they’re going to have a failed ITI. We know male sperm counts are down and have declined by over 50%. We did a study that shows that FemaSeed ITI is beneficial over IUI, even for those with low sperm count.
We ran an FDA-approved prospective study, and we have published peer-reviewed data. We took what we deemed the most challenging patient population – those with low sperm count – because up until ITI, someone with low sperm count only had the option to go to IVF or ICSI. We asked, knowing that we put the sperm right there, do we overcome that challenge? And we achieved a 26.3% pregnancy rate by subject (Journal of Gynecology & Reproductive Medicine). That’s quite high. It’s more than double what is seen with IUI, and again, in a challenging patient population.
Though there are no guarantees, ITI is the least invasive and most effective first step. In my view, this is a replacement to the traditional, old, antiquated IUI. This is not a replacement to IVF, which involves many other things, but this step is really easy to understand: the sperm needs to get to the tube to fertilize the egg, and that’s what FemaSeed achieves.
I founded this company 22 years ago. I’m so excited by this moment in time – we have the opportunity to help patients have the families they desire, whatever that looks like. That’s what keeps me going every day.
I think about how many accolades I get as a pioneer and a founder, but my greatest gift is being a mom. If I can bring that gift to others, there’s nothing that brings me greater joy. So if patients go and ask for technology and advocate for themselves, they can ask for FemaSeed ITI, and they should be able to be granted that. Women should advocate for themselves. Go get it. We will be there to help. This is the moment where we change the course of how we handle fertility journeys – giving people earlier access, lower cost, and lower risk options to achieve their families.”
After IUI Failures and Loss, How Aslyn Found Success with FemaSeed
Aslyn, a FemaSeed patient with a powerful journey, opens up about what the ITI procedure really feels like, and how it ultimately led her to a successful pregnancy.
“My partner and I had been trying to conceive, and we had gotten pregnant naturally twice. Unfortunately, the first pregnancy ended in an ectopic pregnancy and the second ended in a miscarriage, which was really difficult for us both. We decided to try some fertility treatments this past summer. We started with medication alone, then did a cycle of IUI, which didn’t work out for us.
After losing our first two, we definitely felt lost and a bit hopeless, and unfortunately lacked the financial means for IVF. Once we discovered FemaSeed and realized we could afford to try it a couple of times, we finally felt a little hope. For us, the success rates were about the same as IVF for my age, so it gave us great hope knowing that we might get lucky trying something much more affordable and less invasive.
We honestly heard about the treatment from a friend who had just heard of it themselves and thought, ‘Why not give it a try?’ We were the third couple to ever receive the treatment at our clinic. Wild! The first time we did it, it was a little bit painful but everyone, including ourselves, were learning. The second time, our NP at CNY Fertility knew how to calm me and used some topical lidocaine to make me more comfortable. It was much easier on my body.
It honestly wasn’t until we got the positive pregnancy test that we knew for sure that things had worked out. We had experienced so much loss and so many failures that we were in a bit of a defeated mode, but we were so incredibly thankful to know it worked.”
A Fertility Doctor on the Limits of IUI – and What Comes Next
For many patients, the hardest part of IUI isn’t just the outcome – it’s the uncertainty of how effective it may be. To unpack what’s really happening behind the scenes, we spoke with Dr. Carrie Bedient, MD, FACOG, a reproductive endocrinologist at The Fertility Center of Las Vegas and co-founder of Fertility Docs Uncensored. From her perspective in the clinic, she’s seen firsthand where IUI can fall short – and why more precise, modern options are gaining attention.
“The most common misconception from patients who are undergoing IUI is that it’s going to work every time. Even in the best case scenario where we have an ovulating egg, open tubes, an adequate sperm count, and a thick endometrium, the odds of success remain very low. In the absolute best case scenario, success rates are about 15%. This means that over 85% of the time we are calling patients with negative pregnancy tests at the end of their two week wait. The anguish in their voice is very real as they question why it didn’t work when all of the parts and pieces seemed to be in place. Frustration follows shortly thereafter as they do multiple cycles of a treatment with a very low success rate and begin to burn out mentally and emotionally.
From a physician’s perspective, FemaSeed removes the opportunity for sperm to get lost on its way to the egg. With a traditional IUI, you have successfully bypassed the barrier of the cervix, but the sperm still have a huge amount of distance to cover through the uterine cavity on their way to the tubal opening. Additionally, half the sperm are going to enter the wrong tube that doesn’t have an ovulated egg waiting. An ITI bypasses the cervix and the uterine cavity and places all available sperm right at the entrance to the tube, maximizing its ability to reach the egg. Anyone who is working with a very low sperm count may benefit from ITI because it doesn’t require the higher total motile sperm counts needed for IUI. Patients who formerly would’ve had no choice but in vitro fertilization now may have the option of trying ITI.
A few different types of patients can be really good candidates for ITI. Anyone who is working with a very low sperm count may benefit from ITI because it doesn’t require the higher total motile sperm counts needed for IUI. Patients who formerly would’ve had no choice but in vitro fertilization now may have the option of trying ITI. Women with only one functional two may also benefit by ITI because all this sperm can be directed towards the one place it needs to go. Couples using donor sperm may also benefit from ITI because the success rate is higher, minimizing the number of vials they will have to purchase. And of course, anyone who is looking for the most efficient way to get pregnant, but is not ready to jump immediately to IVF, would benefit from one or two cycles of FemaSeed.
The most meaningful difference that FemaSeed has made in practice is the ability to speed up the whole treatment process. Many patients get stuck in a vicious cycle of ‘one more month’ of timed intercourse or IUI. They hope that these treatments with very low success rates will work, and in the process they get progressively more frustrated, angry, depressed, and tired, necessitating breaks from treatment. The upshot is that doing multiple cycles of a minimally successful treatment and then needing to pause treatment to collect yourself can delay more effective treatments by a year or more. At that point, increasing age worsens the prognosis and the path to parenthood gets even steeper. My patients who are able to do FemaSeed have a much more direct, smooth path to building their family. I think it also gives patients a sense of relief to know they can try the less invasive, less expensive treatment, even when they may have only one tube or a very low sperm count. The ability to try more natural cycles gives many couples a sense of relief that they are doing everything they can to build their family.”
Innovation in Fertility Is Giving Patients More Hope Than Ever
At a time when fertility journeys are defined by uncertainty, repetition, and emotional strain – and too often constrained by cost – innovations that improve outcomes while increasing access offer something meaningful.
What makes approaches like ITI so compelling isn’t just the potential for improved outcomes – it’s the shift toward more intentional, data-driven care earlier in the process. For patients who have long felt stuck between ‘wait and see’ and jumping straight to IVF, this evolution signals something meaningful: that the system is beginning to catch up to their needs, their timelines, and their lived experiences.
And with that progress comes something even more essential: hope. Not the kind rooted in blind optimism, but the kind built on new possibilities, better tools, and stories like Aslyn’s that remind us what’s at stake. Innovation in fertility isn’t just about science; it’s about expanding access to care, reducing burden, and giving people more ways to move forward. Because for anyone navigating this path, hope isn’t a luxury – it’s a necessity. And increasingly, it’s one that science is finally learning how to support.

This article is sponsored by Femasys, a women’s health company focused on expanding access to more affordable, less invasive fertility treatment options. Through innovations like FemaSeed®, a targeted insemination approach designed to deliver sperm closer to the fallopian tubes, Femasys is reimagining what first-line fertility care can look like. By offering a procedure that can be performed in-office without the need for more intensive interventions, FemaSeed aims to provide patients with an option that bridges the gap between traditional IUI and IVF. If you’re exploring your options, ask your doctor whether FemaSeed is available at your clinic and whether it could be a fit for your fertility journey. Learn more at femaseed.com

Listen to stories, share your own, and get feedback from the community.